Written by DAN Staff
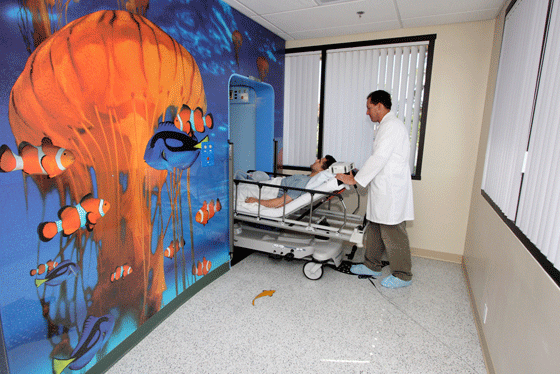
As a dive professional you’re trained to identify and respond to emergencies. Being able to get an injured diver to the surface and out of the water, then provide first aid while arranging for emergency medical care is incredibly important. What happens after the ambulance pulls away, however, is rarely covered and can lead to questions among divers and dive pros. Here’s a look at what occurs when an injured diver arrives at a hyperbaric chamber.
Patient Intake
Most of the time a hyperbaric chamber facility will not (and should not) be the first stop. While minimizing the time to recompression is important, post-dive symptoms require a comprehensive evaluation by a physician to identify any life-threatening issues that may contraindicate recompression.
Once evaluated by an emergency physician, the diver is sent to a hyperbaric chamber. The doctor or chamber staff will conduct a brief physical exam and record a medical history. During this process, it’s important for the staff to get as much information as possible including:
- An honest and thorough description of symptoms and events leading up to the injury.
- The number of dives made over the past few days, along with depths, times and the gases breathed. Sending the diver’s dive computer can help provide additional background.
- Any rapid ascents, omitted decompression or other issues.
Physical and Neurological Exams
After the initial evaluation, the doctor will perform physical and neurological exams to identify any abnormalities that may need further care. These exams will likely focus on the ears, lungs, heart, skin and neurological function. The ears will be checked for visible damage to the eardrum and blood or other fluids. Listening to the heart and lungs can help detect concerns, and any rashes that may be suggestive of decompression sickness (DCS) will be identified. A neurological exam helps determine if there is any impairment indicative of DCS or other problems.
Diagnosis and Additional Testing
After a thorough workup, the doctor can tailor treatment to the injury. Data acquisition allows the doctor to create a differential diagnosis, which is a diagnosis resulting from the patient’s history, identification of abnormalities during exams and data gathered from other physical exams and observations. A differential diagnosis differs from a traditional clinical diagnosis due to the fact that DCI can be exceptionally difficult to diagnose and definitive test results are sometimes not possible to obtain.
A differential diagnosis may indicate the need for additional testing and intervention. Vital sign and pain monitoring, blood tests and metabolic panels to check for organ function are relatively common if symptoms are serious. The doctor may also call for a chest X-ray to rule out pneumothorax before treatment. In serious cases of DCI, additional tests may include electrocardiograms, CT scans and ultrasounds.
Treatment
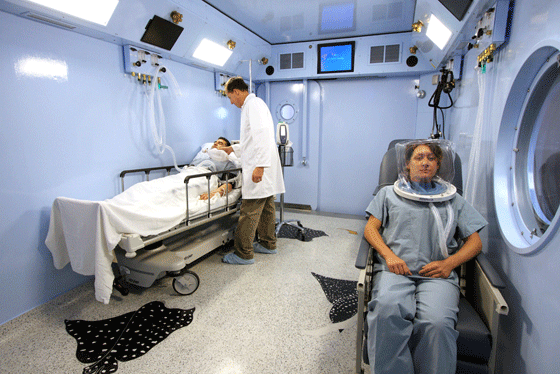
If the diagnosis confirms DCS or arterial gas embolism (AGE), and there are no contraindications to hyperbaric treatment, it’s likely that hyperbaric therapy will be indicated. The general process involves administration of 100 percent oxygen during compression in a hyperbaric chamber. Not all diving-related conditions warrant recompression therapy, and it can exacerbate some injuries (such as pneumothorax), but is otherwise relatively safe and effective at resolving symptoms.
Treatment may involve multiple sessions in a hyperbaric chamber along with many of the same exams performed again. Results provide information about symptom resolution and determine whether the doctor needs to prescribe additional interventions or clear the diver for post-treatment rehabilitation. Depending on the severity of symptoms, the diver will either be sent home to rest with instructions for follow-up and eventual return to diving, or in very severe cases, admitted to the hospital for additional treatment of persistent symptoms or those requiring interventions other than hyperbaric oxygen therapy.
For more information on treating injured divers, visit DAN.org/Health or contact DAN Medical Services at DAN.org/Contact.